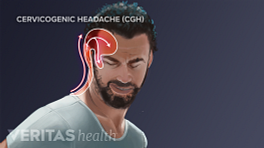
A headache can be caused by a problem in the neck. What we call that is cervicogenic headache. Now most of the time, cervicogenic headaches and let me take a step back and say that most of the headaches do not come from the neck, most of the headaches have a different source, but there is a very specific type of a headache that is called cervicogenic headache stemming from the cervical spine - or in other words, the neck.
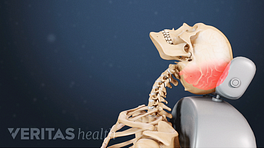
Cervicogenic headache usually starts in what we call the suboccipital area, which is the area — that muscular area that is just under the occiput or the head. That pain tends to start there - it can be on one or both sides - and it tends to radiate up into the head and around the head. The easiest way to visualize it is to actually take the palm of your hand and place it on the back of the head and that really is where the pain spreads. More rarely, the pain can actually travel to the front of the head and behind the eye. Now once again, that's not common and even more - even less common is for it to just appear in the front of the head or behind the eye, but it does happen.
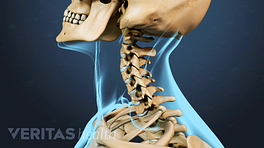
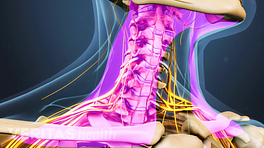
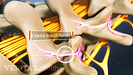
In order to discuss the causes of cervicogenic headache, I need to take a step back for a second and talk about the anatomy. What we're looking at here is the back of the head, the neck or cervical spine, and specifically what we're looking at is these little joints. Now these are facet joints - or zygapophysial joints – hinge-like joints in the spine. Now, these joints are true joints - in other words, they have the synovial fluid, synovial capsule, cartilage - and they can react like any other joint; in other words, they can get irritated, inflamed, and can become painful. Now, what's important in this context is that the innervation for these joints comes from a very small branch - called medial branch - that comes around here and goes into the joint. At times, that branch continues on and goes and becomes another nerve. The nerve that we're concerned about specifically is called the third occipital nerve. This nerve crosses the C2-3 facet joints and the facet joints are named for the different vertebral bodies that are interfacing and forming that joint, so this is a C2 and C3. So a C2-3 joint is crossed by the third occipital nerve, that then continues onto the occiput and up and around the scalp. If there is irritation at this joint, this nerve tends to transmit pain and cause the pain that we're discussing - the pain that actually encompasses the occiput and the back of the head.
Now, the causes of this, there are many to discuss. If we are to group them together, the most common cause is really similar to a whiplash injury. If you think about the joint, the joint itself as a hinge-like joint that provides the sliding motion. Whiplash is essentially acceleration-deceleration injury grinding that joint. That usually is the first step to precipitating this cervicogenic headaches because it irritates the joint, and then the irritation drives the whole process.
Now, whiplash or acceleration-deceleration injury through that joint can mean motor vehicle accidents, can mean just falls - commonly falls on ice - that cause this motion of the head and that's usually more common in the younger population. When we talk about the older population and when the arthritis becomes more of a problem, that arthritis in that same joint can also cause irritation, inflammation, and irritation to that nerve, causing those cervicogenic headaches. Of course, anything that would cause irritation to that nerve can cause the headaches and muscle spasms, grinding that joints, irritation to the joint from other causes, from the laxity of the joint, in different conditions that really predispose the hypermobility or increased mobility of that joint can also predispose to inflammation and irritation of that nerve, once again predisposing to the - one to cervicogenic headaches.
Diagnosing cervicogenic headache can be somewhat tricky because the headaches resemble a number of different headaches and to complicate the matter, they can trigger other headaches. So, for instance, patients can have cervicogenic headaches as another trigger for a migraine. Cervicogenic headaches in itself can cause tension type of headache. But if there is suspicion for cervicogenic headache, the studies have shown that a very precise diagnostic procedure can be very, very accurate in diagnosing it.
The way this procedure is done is under controlled conditions and the guidance of an radiofrequency rhizotomy. Radiofrequency rhizotomy essentially eliminates those feeding nerve fibers and the way this is approached is a probe is placed along the path of this nerve and then radiofrequency energy is used in order to treat this area to eliminate those nerve fibers.
Besides using these techniques, what's important to remember is that cervical manipulations in a gentle manner addressing the actual myofascial component (muscles, connective tissue of the neck) is very, very important as well. So, it‘s important to really address this from a point of view of pain, controlling the pain because, as we know, pain really drives a lot of the muscular spasm and prevents one from doing the exercises and manipulations that are necessary in order to get better. And at the same time, it’s important once that is taken care of, it’s important to have the patient follow up in a very structured physical therapy program that addresses strengthening, postural adjustments, as well as manipulations of myofascial structures and really addressing the muscular tensions around the head. Once everything comes together and all of the components of the biomechanical chain are treated, the myofascial component is treated, the inflammation and irritation is eliminated, and if necessary those offending nerve fibers are eliminated, most patients tend to recover very, very well, especially those that had this cervicogenic headache as a trigger for other types of headaches that are really debilitating.