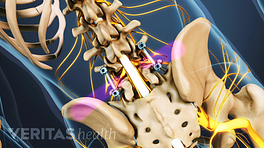
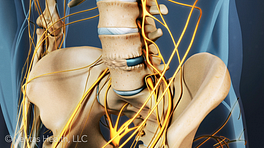
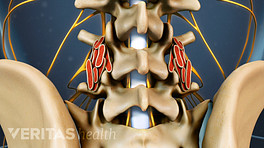
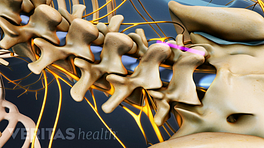
After a posterolateral gutter spine fusion, the body engages in a natural process to repair itself, which usually means growing bone. As the harvested bone graft grows and adheres to the transverse processes, such as between L4 and L5 (lumbar segment 4 and lumbar segment 5), the spinal fusion is achieved, and motion at that segment is stopped.
Medical devices (such as pedicle screws, cages and other spine surgery instrumentation) are sometimes used as an adjunct to obtain a solid fusion. However, a solid fusion is not always achieved.
Risk Factors for Achieving a Solid Spinal Fusion
There are two types of bone cells, one (osteoblast) that grows bone and another (osteoclast) that removes bone. It is a race between these two cell types for the spine fusion to set up successfully.
There are a couple of key factors that patients can control that are important in determining whether or not a fusion grows in solidly, including:
- Smoking cessation. It is generally advisable to quit smoking prior to a spinal fusion surgery, as nicotine is a direct toxin to bone graft and will prevent the bone from forming.
- Limited motion. Bone forms better if motion is limited, so patients are advised to avoid bending, lifting, and twisting for three months after spinal fusion surgery.
Other Considerations for Obtaining a Solid Fusion
Most spine fusions will set up within three months and continue to get stronger for one to two years. Once a solid fusion is achieved, it is very unlikely that it will ever break. Recurrent pain after a successful spine fusion surgery is generally not from the fused level, but can be from any of the other joints.
In This Article:
- Posterolateral Gutter Spine Fusion Surgery
- After Posterolateral Gutter Fusion Surgery: Risks and Complications
- Posterolateral Gutter Fusion Surgery Video
A "transfer" lesion where an adjacent segment breaks down can occur especially if more than one level is fused. A transfer lesion is the result of increased stress being transferred to the next level.
Although transfer lesions have been well documented in multi-level spine fusions, it is less clear if doing a one level fusion leads to a higher incidence of joint breakdown than in the general population (than for people who have not had a spine fusion surgery).
Risks and Complications with Posterolateral Gutter Fusion
The principal risk of this type of back surgery for the lumbar spine (lower back) is that a solid fusion will not be obtained (nonunion), and further surgery to re-fuse the spine may be necessary. Nonunion rates of between 10% and 40% have been quoted in the medical literature.
See Failed Spinal Fusion Surgery
Nonunion rates are higher for patients who:
- Have had prior surgery
- Smoke or are obese
- Have multiple level spine fusion surgery
- Have been treated with radiation for cancer.
Not all patients who have a nonunion will need to have another fusion procedure. As long as the joint is stable, and the patient's symptoms are better, more back surgery is not necessary.
Other than nonunion, the risks of a spinal fusion surgery include infection or bleeding. These complications are fairly uncommon (approximately 1% to 3% occurrence).
In addition, there is a risk of achieving a successful fusion, but the patient's pain does not subside.